Health
Wealthy Nations Can Draw Lessons from Ireland’s Healthcare Transformation

Highlights
- Ireland is changing its healthcare system, moving from American insurance to a UK-inspired universal approach.
- Dublin has the money and political will for this major shift.
- The current two-tier system is inefficient, with almost half relying on private insurance covering just 12% of costs.
- Sláintecare, introduced in 2017, aims for a universal healthcare system by 2030, prioritizing clinical needs.
- Success depends on transitioning staff; 16,200 recruited by 2022, plans for 1,000 more consultants by 2030.
- If successful, Ireland’s model could be a blueprint for countries facing rising health costs and aging populations.
- Challenges in replication include needing political will and financial resources, estimated at around 20 billion euros or 3% of GDP in the first decade.
- UK’s NHS challenges highlight potential risks; Ireland faces similar aging population and staffing challenges.
- Globally, countries are watching Ireland’s shift for insights into a healthier future.
In a groundbreaking move, Ireland is undergoing a major overhaul of its healthcare system, transitioning from an American insurance model to a UK-inspired universal approach. Despite the boldness and expense of this endeavour, Dublin boasts both the financial resources and political will necessary for such a transformative change. As Ireland pioneers this shift, other nations contemplating similar radical reforms must possess fiscal strength and secure public consensus for a successful operation.
Dating back to 1957, Ireland has operated a two-tier healthcare system, where ordinary citizens availed free public services, while a state-backed insurer, VHI Healthcare, covered the top 15% of earners for a fee. However, the system has proven inefficient, with nearly half the population now relying on private insurance, covering only 12% of healthcare costs. This has led to increased feelings of inequality, longer waiting times for those without insurance, and nearly 500,000 people surpassing government-mandated waiting times in 2023.
To address these issues, Dublin introduced “Sláintecare” in 2017, a plan set to be implemented by 2030. This ambitious initiative aims to establish a universal healthcare system, ensuring free delivery of services to all patients based on clinical needs. Key measures include reclaiming beds in public hospitals from private insurers, expanding capacity, and potentially reducing pharmaceutical expenditures through enhanced state negotiating power.
The success of Sláintecare hinges on transitioning medical staff from the private to the public healthcare system. By the end of 2022, over 16,200 staff, including nurses, doctors, and other professionals, were recruited, with plans to hire an additional 1,000 consultants by 2030. This concerted effort, coupled with competitive wages, is crucial for ensuring a smooth transition.
Ireland’s Healthcare Revolution: A Blueprint for Universal Reform
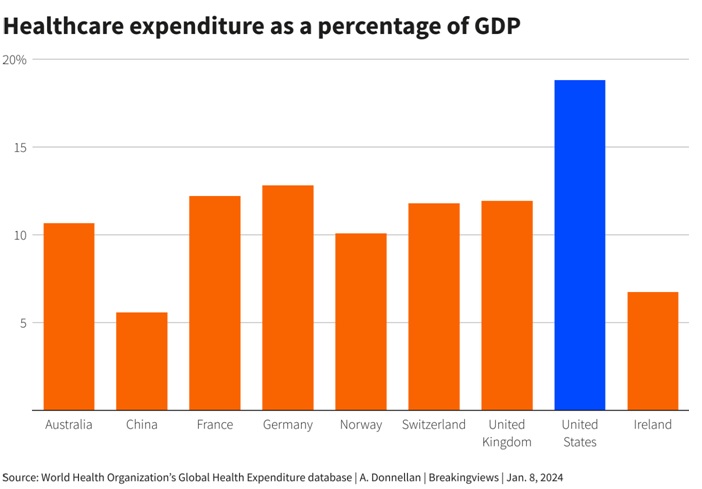
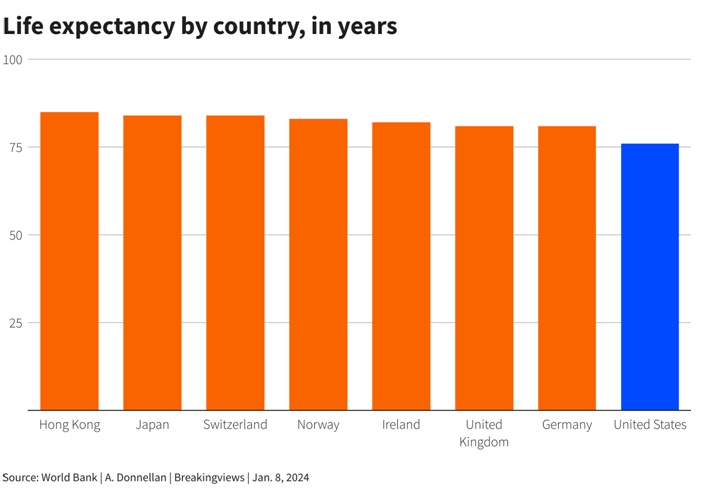
If Sláintecare proves successful, it could serve as a model for other countries with insurance-focused systems grappling with rising health costs and aging populations, such as Germany. The United States, with its substantial healthcare expenditure of 19% of GDP, could also draw valuable lessons from Ireland’s experiment, especially considering disparities in life expectancy and maternal and infant mortality rates.
However, replicating Ireland’s ambitious plans requires two essential ingredients. First, political will, as witnessed in Ireland with support from all major political parties forming a cross-party parliamentary committee. This contrasts with the deeply polarizing issue of healthcare funding in the U.S., compounded by a powerful insurance lobby.
Secondly, financial resources are critical, with Sláintecare estimated to cost around 20 billion euros or 3% of Ireland’s GDP in the first decade. While Ireland currently enjoys a surplus derived from U.S. multinationals benefiting from low corporate tax rates, the U.S. faces a more challenging financial scenario with a significant budget deficit.
Ireland’s Healthcare Revolution: A Blueprint for Universal Reform
Cautionary tales, such as the challenges faced by the UK’s NHS due to decades of under-investment, underscore the potential risks of such healthcare transformations. Ireland, like the UK, grapples with an aging population and the need for skilled staff, a challenge exacerbated by the pandemic-induced exodus of workers.
As the U.S. and other countries confront escalating healthcare costs and the lasting impact of COVID-19, they observe Ireland’s healthcare makeover with a blend of envy and hope. While the road to universal reform is fraught with challenges, Ireland’s bold steps may offer valuable insights for a healthier future.





















































